Navigating the Brain with Precision
Consider the challenge of traversing an unfamiliar city without a map—relying solely on intuition to avoid dead ends and critical intersections. Now envision that city as the human brain, where I, as a neurosurgeon, must navigate past a tumor without disrupting the pathways that define a patient’s ability to speak, move, or think. This is where tractography becomes indispensable, serving as my navigational tool within the intricate landscape of the brain.
In my practice, this advanced technology transforms the daunting task of tumor resection into a meticulously planned procedure, ensuring both safety and efficacy. Allow me to guide you through the remarkable role of tractography in addressing brain tumors, revealing how it enhances surgical outcomes with unparalleled precision.
Understanding Tractography: A Window into Brain Connectivity
Tractography is a sophisticated imaging technique that provides a detailed view of the brain’s white matter tracts—the fiber bundles that transmit signals between different regions. The brain houses approximately 86 billion neurons, each communicating through these tracts, which function as the organ’s communication network.
While a standard MRI offers a static image—useful for identifying a tumor’s location—it lacks the ability to reveal these underlying connections. Tractography, derived from diffusion tensor imaging (DTI), a specialized MRI method, addresses this limitation. By tracking the movement of water molecules along these fibers, it generates a three-dimensional, color-coded map—red indicating left-to-right pathways, blue for vertical, and green for anterior-to-posterior. This map equips me with a comprehensive blueprint, enabling precise planning for tumor surgery.
The Critical Role in Tumor Resection
Brain tumors frequently position themselves near essential functional areas, such as those responsible for speech or motor control, posing a significant challenge during surgery. Removing too much tissue risks impairing a patient’s abilities, while leaving tumor remnants may allow regrowth. Tractography mitigates this dilemma by delineating the tumor’s boundaries alongside vital white matter tracts—such as the corticospinal tract, which governs movement, or the arcuate fasciculus, crucial for language.
Recently, I encountered a case involving a tumor adjacent to the speech fibers in a patient’s left posterior temporal region. Tractography provided a clear visualization of the areas to avoid and those requiring careful navigation during resection. This precision enabled us to excise the tumor without compromising the patient’s capacity to produce or comprehend speech—a testament to tractography’s transformative impact.
Application in the Operating Room
Prior to surgery, I review the DTI scans, which present a detailed three-dimensional representation of the patient’s brain connectivity. This preparation phase is akin to studying a topographic map before a complex journey—identifying the tumor’s location and plotting a route that preserves critical pathways. In the operating room, this map is integrated into advanced navigation systems, such as Brainlab or StealthStation, displayed on a monitor beside me.
As I proceed with the resection, the system overlays real-time visuals, guiding my instruments with exactitude—akin to receiving continuous updates from a navigation device: “In two millimeters, steer clear of the language pathway.” This technology ensures that each incision is calculated, preserving the patient’s neurological function while addressing the tumor comprehensively.
Evidence of Efficacy: Improved Patient Outcomes
The benefits of tractography are substantiated by recent research. A 2024 study published in the Journal of Neuro-Oncology demonstrated that its use in glioblastoma surgery—a particularly aggressive tumor type—improved survival rates by facilitating more complete tumor removal, with some cases showing up to a 20% enhancement in outcomes. Additionally, a report from Neurosurgery in the same year indicated a significant reduction in postoperative deficits, such as speech or motor impairments, when tractography was employed.
My own experience aligns with these findings: the successful preservation of speech in my recent patient underscores the practical value of this tool in achieving favorable results. Such data resonates beyond the medical community, as evidenced by online discussions noting its life-saving potential.
The Technology Behind the Maps
The foundation of tractography lies in DTI, which captures the diffusion of water molecules along axonal pathways—the structural cables of white matter. Advanced computational algorithms then translate this data into a vivid, three-dimensional model, accessible through intraoperative navigation platforms. These systems synchronize preoperative imaging with the surgical field, offering a dynamic view of the tumor and surrounding tracts.
This integration enhances my ability to execute precise interventions, ensuring that critical functions remain intact. The visual appeal of these models—often likened to a vibrant network—captures public interest, highlighting the intersection of technology and medicine in modern neurosurgery.
Advancements on the Horizon: The Role of Artificial Intelligence
Looking forward, tractography is poised for further evolution, particularly with the integration of artificial intelligence (AI). Recent developments, such as MIT’s 2025 trials in automated fiber segmentation, demonstrate AI’s capacity to refine these maps with greater accuracy—improving delineation by approximately 15%, according to a January 2025 Nature Neuroscience publication.
This advancement could serve as a virtual assistant, alerting me to subtle shifts in fiber orientation near a tumor. Future iterations may combine tractography with robotic surgical systems, enabling resections of unprecedented precision. Such innovations promise to elevate this technology, enhancing its utility in the fight against brain tumors.
Relevance to the Public
The significance of tractography extends beyond the operating room, touching lives in tangible ways. For individuals affected by brain tumors—whether a family member with glioblastoma or a friend recovering from neurological trauma—this technology offers hope through improved surgical precision and better outcomes.
In my practice, I witness its impact firsthand: one patient, an artist, retained her ability to create following surgery, thanks to careful mapping of her motor pathways. Beyond tumor management, tractography informs treatments for conditions such as stroke, epilepsy, and Parkinson’s disease, broadening its relevance. It exemplifies how advancements in neurosurgery translate into restored capabilities and extended quality of life.
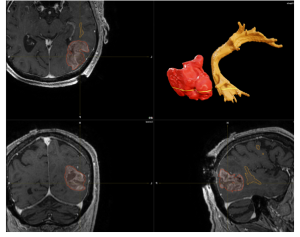
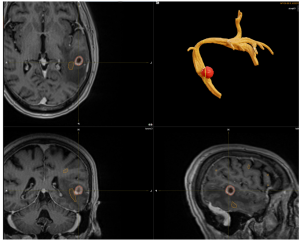
Figure 1 and 2: Multimodal Imaging of a Brain Tumor with Language White Matter Pathway
This composite image illustrates a brain tumor using multiple imaging modalities. The top left, bottom left, and bottom right panels display MRI scans of the brain in axial, coronal, and sagittal views, respectively. The tumor is highlighted in red, and the language pathway boundaries outlined in yellow, showing their location and extent within the brain tissue.
The top right panel presents a 3D reconstruction of the tumor (in red) and a tractography 3D reconstruction of the language white matter pathway (in yellow), providing a detailed visualization of the tumor’s spatial relationship with the critical language pathways. This multimodal approach aids in understanding the tumor’s impact on language function and planning potential surgical or therapeutic interventions.
Conclusion: Precision as a Pathway to Recovery
Tractography represents a cornerstone of modern neurosurgery, providing a detailed navigational framework for addressing brain tumors with accuracy and care. From preserving speech in my recent case to enhancing survival rates across studies, it empowers surgeons to achieve outcomes once deemed unattainable. As artificial intelligence and other technologies enhance its capabilities, tractography stands as a beacon of progress in our field—mapping not just the brain, but a future where patients reclaim their lives.